Exploring Mosquito-Borne Diseases In the U.S.
All of the data points in this post were obtained from the Center for Disease Control (CDC)’s website as of 02/13/2018.
West Nile Virus (WNV)
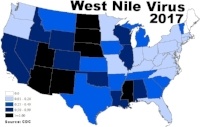 47 out of 50 states and the District of Columbia have reported West Nile virus infections in people, birds, or mosquitoes in 2017. Overall, 2,002 cases of WNV were reported in humans, and there were 121 (6%) confirmed deaths in 2017. While this data shows a decrease in the number of human cases reported in 2016 (2,149), it also brings attention to the increase in lives lost, when compared to the 106 (5%) confirmed deaths in 2016. The states reporting the highest number of WNV disease cases* in 2017 include:
47 out of 50 states and the District of Columbia have reported West Nile virus infections in people, birds, or mosquitoes in 2017. Overall, 2,002 cases of WNV were reported in humans, and there were 121 (6%) confirmed deaths in 2017. While this data shows a decrease in the number of human cases reported in 2016 (2,149), it also brings attention to the increase in lives lost, when compared to the 106 (5%) confirmed deaths in 2016. The states reporting the highest number of WNV disease cases* in 2017 include:
Texas: 133 cases, 5 deaths
Georgia did not report as many WNV cases (47) as several other areas of the country; however, the state reported one of the highest numbers (7) of confirmed lives lost as a result of the virus.
*Numbers combine Neuroinvasive Disease Cases and Non-neuroinvasive Disease Cases
WNV is typically transmitted to humans by mosquitoes that have previously fed upon an infected bird. While over 150 species of mosquitoes have been known to carry WNV, the main vector species in the U.S. are Culex pipiens, Culex tarsalis, and Culex quinquefasciatus. These mosquitoes are all active at night, and most cases of infection occur during the summer months. Approximately 20% of people affected by WNV will experience flu-like symptoms including fever, headache, nausea, muscle pain, and swollen lymph glands. Other symptoms may include a stiff neck, rash, sleepiness or disorientation. Less than 1% of those infected will develop West Nile Encephalitis or Meningitis, which can lead to coma, tremors, convulsions, paralysis, and even death.
To learn more about the symptoms, treatment, and mosquito species that vector this virus, visit our educational page on West Nile virus.
Eastern Equine Encephalitis (EEE)
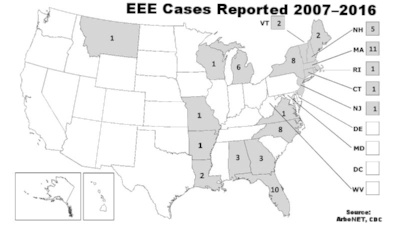 Eastern equine encephalitis, also referred to as EEE or Triple E, is a rare but deadly illness for humans. Thankfully, only a few human cases of EEE are reported in the U.S. each year. The CDC sites that an average of 7 cases of EEE were reported annually in the U.S. from 2007 – 2016. In 2016, there were 7 reported human cases of EEE and 3 of those cases were fatal. As of January 9, 2018, there were 3 human cases of EEE reported to the CDC in 2017.
Eastern equine encephalitis, also referred to as EEE or Triple E, is a rare but deadly illness for humans. Thankfully, only a few human cases of EEE are reported in the U.S. each year. The CDC sites that an average of 7 cases of EEE were reported annually in the U.S. from 2007 – 2016. In 2016, there were 7 reported human cases of EEE and 3 of those cases were fatal. As of January 9, 2018, there were 3 human cases of EEE reported to the CDC in 2017.
The reason EEE is less common in humans is that the primary mosquito vector (Culiseta melanura), does not typically feed on humans. It is believed that EEE virus is mainly transmitted to humans and horses by bridge vectors that have contracted the virus by feeding on infected birds. Symptoms typically occur four to ten days after a bite from an infected mosquito and include fever, headache, vomiting, muscle aches, joint pain, and fatigue. In rare cases, infection occurs in the brain and spinal cord leading to sudden high fever, stiff neck, disorientation, seizures, and coma. The mortality rate of those that develop EEE is about 33%, the highest among human arboviruses (a virus transmitted by arthropod vectors) cases reported in the U.S. The disease is also a concern for horses. There is a vaccine available for horses, and horse owners are encouraged to discuss an on-going vaccination schedule with their veterinarians. Currently, there is no human vaccine for EEE.
To learn more about the symptoms, treatment, and mosquito species that vector this virus, visit our educational page on EEE virus.
Zika Virus (ZIKV)
 In 2017, within the United States, there were 4 ZIKV cases of local mosquito-borne transmission, 5 cases acquired via sexual transmission, and 409 travel-associated cases reported to the CDC. The 4 local cases were from Florida (2) and Texas (2), the same states that reported the only local cases in 2016 (Florida: 218 and Texas: 6).
In 2017, within the United States, there were 4 ZIKV cases of local mosquito-borne transmission, 5 cases acquired via sexual transmission, and 409 travel-associated cases reported to the CDC. The 4 local cases were from Florida (2) and Texas (2), the same states that reported the only local cases in 2016 (Florida: 218 and Texas: 6).
U.S. Territories reported a total of 636 local cases in 2017, a dramatic decrease from the previous year. In 2016, U.S. Territories reported close to 36,000 cases of Zika virus that were likely acquired through local mosquito-borne transmission. VDCI partnered with the CDC in several U.S. territories in 2016 to help combat the spread of Zika virus.
Many individuals learned about Zika during the outbreaks in South and North America; however, the virus was first discovered in 1947 in the Zika Forest of Uganda. In the Americas, it has only been linked to transmission by Aedes aegypti or the Yellow Fever mosquito. Ae. aegypti is also responsible for the transmission of dengue virus, yellow fever virus, and chikungunya virus. In Africa, the virus was detected in Aedes albopictus or the Asian tiger mosquito; hence, it is possible that Ae. albopictus could vector the virus in the Americas.
When symptoms occur, they typically begin with a mild headache and fever. Within a day or two, a maculopapular rash may appear and can cover many parts of the body. Following the rash, people generally report continued fever, malaise, and body aches. Other symptoms can include diarrhea, constipation, abdominal pain, and dizziness. Treatment for symptoms includes hydration, rest, and the use of acetaminophen to relieve fever. If a pregnant woman is infected with Zika virus, it may result in microcephaly, a birth defect causing underdevelopment of the head and brain in newborn children. Currently, there is no vaccine or cure for ZIKV.
To learn more about the symptoms, treatment, and mosquito species that vector this virus, visit our educational page on Zika virus.
Contact Us to Learn More About Effective Mosquito Prevention Strategies:
 Since 1992, Vector Disease Control International (VDCI) has taken pride in providing municipalities, mosquito abatement districts, industrial sites, planned communities, homeowners associations, and golf courses with the tools they need to run effective mosquito control programs. We are determined to protect the public health of the communities in which we operate. Our mosquito control professionals have over 100 years of combined experience in the field of public health, specifically vector disease control. We strive to provide the most effective and scientifically sound mosquito surveillance and control programs possible based on an Integrated Mosquito Management approach recommended by the American Mosquito Control Association (AMCA) and Centers for Disease Control and Prevention (CDC). VDCI is the only company in the country that can manage all aspects of an integrated mosquito management program, from surveillance to disease testing to aerial application in emergency situations.
Since 1992, Vector Disease Control International (VDCI) has taken pride in providing municipalities, mosquito abatement districts, industrial sites, planned communities, homeowners associations, and golf courses with the tools they need to run effective mosquito control programs. We are determined to protect the public health of the communities in which we operate. Our mosquito control professionals have over 100 years of combined experience in the field of public health, specifically vector disease control. We strive to provide the most effective and scientifically sound mosquito surveillance and control programs possible based on an Integrated Mosquito Management approach recommended by the American Mosquito Control Association (AMCA) and Centers for Disease Control and Prevention (CDC). VDCI is the only company in the country that can manage all aspects of an integrated mosquito management program, from surveillance to disease testing to aerial application in emergency situations.

